Herniated Disc
Discs cushion the small bones, known as vertebrae, within the back. These diminutive discs have a tough exterior layer that encompasses the nucleus. The discs absorb shocks from the spinal bones. A disc that herniates, also referred to as a ruptured, slipped, or bulged disc, is a part of the nucleus of the disc that moves out from the annulus into the spinal canal when a rupture or tear that occurs within the annulus.
A herniated disc is almost always in the initial stage of degeneration. The spinal canal’s space is finite, meaning a displaced herniated disc fragment and spinal nerve will not have enough space in this constricted area. The displacement leads to the disc pressuring the nerves within the spine, causing significant pain. Herniated discs have the potential to occur along the entirety of the spine. However, the lumbar portion of the spine, meaning the lower back, is usually the most common site of herniated discs. The cervical section, meaning the neck region of the spine, is also a common site for a herniated disc.
Causes of Herniated Disc
An injury or strain can lead to a herniated disc. Disc material gradually degenerates throughout the aging process. The ligaments that hold the disc in position weaken as time progresses, causing the disc to eventually rupture even with a seemingly minor twisting motion. It must be noted certain patients are particularly likely to suffer from herniated disc issues. One’s genetics play a significant role in the likelihood of a herniated disc.
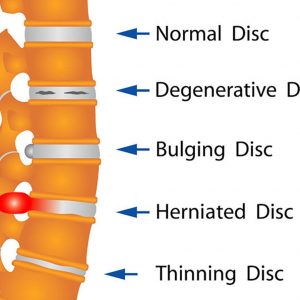
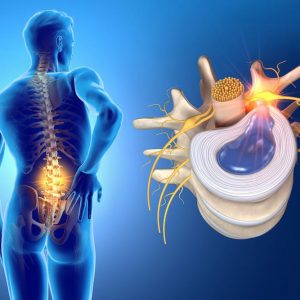
Symptoms of Herniated Disc
The symptoms of a herniated disc are not guaranteed to be the same with every single patient. The magnitude of the herniation along with the disc’s position play a part in determining the symptoms. If the disc does not pressure the nerve, there might be minimal pain or even no pain.
In general, frequent low back pain or a single instance of lumbar pain sets the stage for a herniated disc. If the disc presses against the nerve, there will be weakness, numbness and/or pain. This pain and numbness will move all the way to the body site where the nerve reaches, making life quite difficult due to ongoing pain.
Treating Herniated Disc
The hope is that a herniated disc can be treated without surgical intervention. If a reduction in activity level does not decrease spinal nerve inflammation and reduce the pain, nonsteroidal anti-inflammatory medication will be considered. However, if the pain is significant, an epidural steroid injection with a spinal needle performed under x-ray guidance will transmit the medication to the specific point of disc herniation.
Physical therapy might also be helpful. Some patients suffering from a herniated disc benefit from massage therapy, the application of heat or ice, stretching, pelvic traction and/or electrical muscle stimulation. If necessary, surgery will be considered. However, surgery is a last resort that is only explored if medications, physical therapy, and other treatment modalities do not work.
We are Accepting New Patients
Our pain management doctors are accepting new patients. To schedule an appointment, please call our Carrollton clinic at (972) 316-7270 or our Denton clinic at (940) 222-8943.

